Identify, Specify, Modify: 3 Key Steps for Effective Exercise Prescription

How many times have you found yourself assigning similar exercises to patients with various conditions? Think about how many times you have prescribed basic exercises, such as clamshells or bridges to strengthen the gluteal muscles, without determining whether or not it was the most appropriate exercise.
Therapists can often lose sight of the art of exercise prescription and progression. This article discusses how to develop specialized exercise programs that ultimately lead to helping our patients meet functional goals. We will also discuss the fundamental need for a progressive increase in the challenge of exercise. To get started choosing, modifying, and progressing programs, we can follow the three key steps outlined below.
1. Identify the Primary Impairment
The first step in choosing an exercise that will improve your patient’s activity limitation is to identify their primary limiting impairment. Use objective measures to identify whether the patient’s primary impairment is related to one of the following:
- Mobility deficits – joint or soft tissue restrictions
- Muscle performance deficits – strength, power, or endurance deficits
- Movement coordination impairments – abnormal/aberrant movement patterns, incorrect muscle activation timing, or balance deficits
2. Create Task Specific Exercises
After you’ve identified the primary impairment(s), you’re ready to intervene. You want to provide your patients with exercises that are meaningful and can be replicated at home. Creating exercises that specifically mirror functional tasks has two main benefits:
- Patient understanding – Patients can see the direct link between your exercise prescription and the activities that they want to perform without pain or difficulty.
- Functional carryover – Since the exercise is similar to the activity limitation, you can be more confident that you will see improvements the actual task performance following the prescribed exercise.
Task Specificity Example – Sit-to-Stand
Imagine your patient has limited ankle dorsiflexion during the weight acceptance phase of a sit to stand task. Assessing their ankle mobility reveals limited posterior glide of the talus, the primary impairment restricting their ankle range of motion. You can now use this information to create a task specific self-mobilization that glides the talus posteriorly during sit-to-stand transfers. The video below (provided by Jared Vagy, courtesy of The Athlete Movement System) demonstrates use of a strong elastic band to create posterior mobilization of the talus with a squat. This technique effectively addresses the mobility deficit that was identified as the patient’s primary impairment and mirrors the task of sit-to-stand transfers.
3. Apply Exercise Modifications
Now that you have chosen an exercise that is specific to your patient’s functional tasks, you need to modify the exercise to meet your patient’s skill level. There are 9 main variables that can be adjusted in order to increase or decrease the demand of any exercise. Each variable includes a spectrum of options, leading to countless variations of each exercise. Based on your patient’s performance, you can adjust one or multiple variables, making sure that the patient is able to demonstrate good form with your exercise choice. You may even choose to use one variable to increase the demand of the exercise while simultaneously using another variable to decrease the demand.
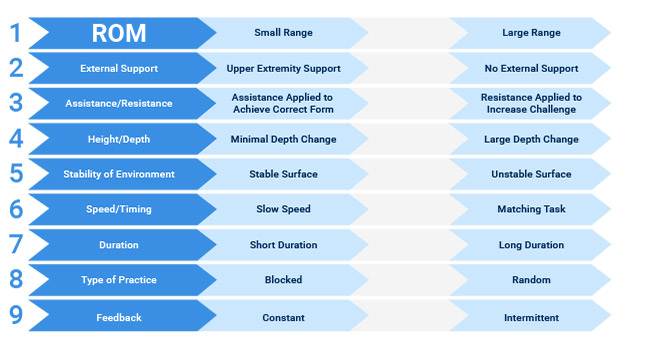

Exercise Adjustment Example – Running (Single Leg Task)
This is one example of a progression for a runner presenting with excessive knee valgus due to excessive hip adduction during a single leg squat. This runner’s abnormal movement pattern is due to hip abductor weakness.
Initial Exercise: Anterior lunge with green Theraband (anchored medially) in front of a mirror.
Variables:
- External support (double leg exercise)
- Resistance (green Theraband)
- Feedback (constant)
- Speed (slow)
Progression 1: Single leg squat with green Theraband and upper extremity support in front of a mirror.
Variables:
- External support (single leg, upper extremity) – increases demand at lower extremity, decreases demand through upper extremity support
- Resistance (green Theraband) – maintain demand
- Feedback (constant) – maintain demand
- Speed (slow) – maintains demand
Progression 2: Single leg squat with red Theraband with no upper extremity support performed quickly with intermittent video feedback.
Variables:
- External support (single leg, no upper extremity support) – increase demand
- Resistance (red Theraband) – decrease demand
- Speed (quick) – increase demand
- Feedback (intermittent) – increase demand
Progression 3: Single leg hop from 4” box with no resistance band with intermittent video feedback
Variables:
- External support (single leg, no upper extremity) – maintain demand
- Resistance (no Theraband) – decrease demand
- Speed (quick) – maintain demand
- Feedback (intermittent) – maintain demand
- Height/Depth (4” box) – increase demand
Progressively Working Toward Goals
Graded exercise programs help patients systematically work toward goals. To design effective progressive programs we should follow these three steps:
- Identify the primary impairment
- Create task specific exercises
- Apply exercises adjustments
Try using these steps, along with your own creativity, to create exercises that bridge the gap between your patient’s current activity limitations and their goals.




