Don’t Be Afraid of Early Mobilization in Acute Brain Injury
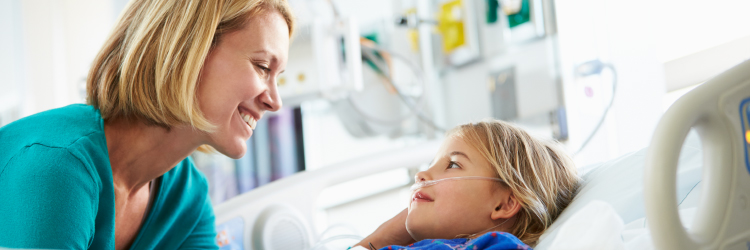
People who suffer brain injuries require extensive medical care to preserve vital organ functions and prevent secondary injury. Physical therapists are in a unique position to positively influence the ultimate outcome for these individuals by simply providing early mobilization.
Evidence
Two studies provide support for early mobilization following brain injury:
- Klein et al examined outcomes of 637 people treated in a neuro intensive care unit and determined that early mobilization did not result in more complications. The study also found that early mobilization led to a shorter stay and earlier discharge.1
- Bartolo et al studied 102 patients admitted to neuro intensive care units following acute brain injury and found high rates of inconsistencies when mobilization was initiated (8 days after admission +/- 8 days) and physical therapy was ordered for only 67% of patients. Referrals to rehab following ICU stays were made for only 60% of patients.2
Sharing these with medical and nursing staff can help achieve the best outcomes for your patients. Unfortunately, the ICU team is not always up to date on this evidence.
What the Evidence Tells Us
As physical therapists, we use evidence-based care to guide our practice in order to achieve the best possible outcomes for our patients. These studies demonstrate that although early mobilization is best practice, approximately 35% of patients are not receiving the best possible care because of delayed mobilization.
What You Can Do
As acute care physical therapists, you need to partner with the physicians, nurses and other therapists in the ICUs. Approach the team armed with evidence to support your physical therapy plan to mobilize patients as early as possible. Once the team shares a common vision of improving outcomes, the practice will become part of the ICU culture in your hospital.
How to Implement
Approach the attending physicians and request referrals for physical therapy for patients following brain injury. Enlist the assistance of nurses and other therapists in managing ventilators, lines, leads and tubes so that you can focus on assisting the patient to standing or transferring to a chair. Keep track of lengths of stay following implementation to support your early mobilization program.
- Klein K et al. Clinical and psychological effects of early mobilization in patients treated in a neurologic intensive care unit: a comparative study. 2015; 43(4):865-73
- Bartolo, M., Bargellesi, S., Castioni, C. A., Bonaiuti, D., Antenucci, R., Benedetti, A., Zucchella, C. (2016). Early rehabilitation for severe acquired brain injury in intensive care unit: Multicenter observational study. European Journal of Physical and Rehabilitation Medicine, 52(1), 90-100.









